Patient Blood Management (PBM) is a patient-centred, systematic, evidence-based approach to improve patient outcomes by managing and preserving a patient’s own blood while promoting patient safety and empowerment. Rather than relying primarily on blood transfusions, PBM focuses on optimising the patient’s own blood health and reducing avoidable blood loss.
The concept has been endorsed internationally, including by the World Health Organization (WHO), which encourages healthcare systems to implement PBM as part of improving patient safety, reducing unnecessary transfusions, and strengthening healthcare sustainability.
Why Patient Blood Management Matters
Blood transfusion can be lifesaving when clinically necessary, but it is also a limited medical resource and carries potential risks, including transfusion reactions, infections, immune complications, and increased healthcare costs. PBM aims to ensure transfusions are used only when truly needed while protecting patient health and outcomes.
Evidence shows that implementing PBM can:
- Improve patient outcomes and reduce complications
- Reduce morbidity, mortality, and length of hospital stay
- Lower healthcare costs
- Preserve blood supplies for patients who truly need them
Because of these benefits, many experts advocate that PBM should be considered a standard of care across healthcare systems.
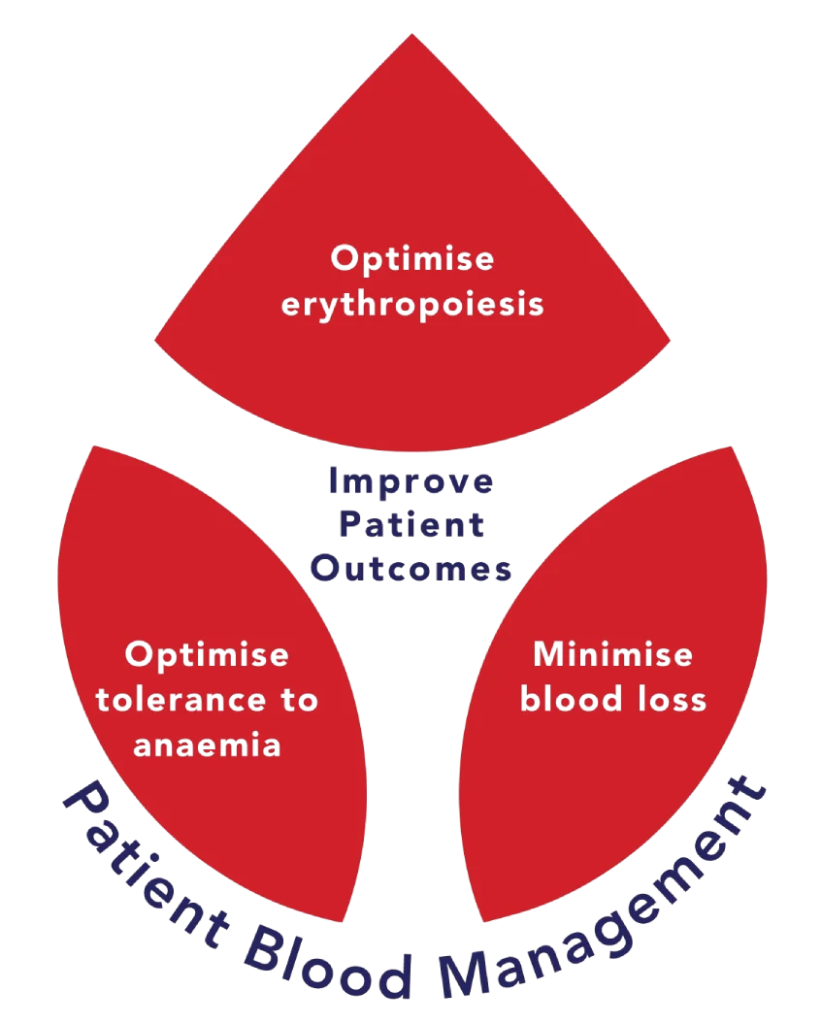
The Three Pillars of Patient Blood Management
PBM is built on three core pillars that guide clinical decision-making throughout a patient’s care journey.
- Detect and Treat Anaemia Early
The first pillar: optimise erythropoiesis, focuses on identifying and correcting anaemia, especially iron deficiency as a step before procedures or during medical care.
Strategies may include:
- Screening for anaemia before surgery
- Treating iron deficiency with oral or intravenous iron
- Addressing underlying medical conditions affecting blood production
Optimising haemoglobin levels before treatment significantly reduces the likelihood of transfusion and improves recovery outcomes.
- Minimise Blood Loss
The second pillar focuses on preventing and controlling bleeding during medical treatment or surgery.
Examples include:
- Using minimally invasive surgical techniques
- Careful surgical planning and haemostasis
- Use of medications that reduce bleeding
- Limiting unnecessary blood draws
- Reducing blood loss directly decreases the need for donor blood transfusions.
- Optimise the Patient’s Tolerance of Anaemia
The third pillar involves improving the body’s ability to tolerate lower haemoglobin levels safely and ensuring transfusions are only given when clinically necessary.
This may involve:
- Restrictive transfusion thresholds
- Optimising oxygen delivery and circulation
- Individualised patient monitoring
By carefully evaluating when transfusions are truly required, clinicians can avoid unnecessary exposure to blood products.
References:
World Health Organization. The Urgent Need to Implement Patient Blood Management: Policy Brief. Geneva: World Health Organization; 2021. Available from: https://iris.who.int/handle/10665/346655
World Health Organization. Action Framework to Advance Universal Access to Safe, Effective and Quality-Assured Blood Products 2020–2023. Geneva: World Health Organization; 2020. Available from: https://www.who.int/publications/i/item/9789240000384
National Blood Authority Australia. Patient Blood Management Guidelines. Canberra: National Blood Authority; 2012–present. Available from: https://www.blood.gov.au/pbm-guidelines
Shander A, Hofmann A, Ozawa S, et al. Activity-based costs of blood transfusions in surgical patients at four hospitals. Transfusion. 2010;50(4):753–765.
Gombotz H. Patient Blood Management: A patient-oriented approach to blood replacement with the goal of reducing anemia, blood loss and transfusion. Transfusion Medicine and Hemotherapy. 2012;39(2):67-72. doi:10.1159/000337833
Meybohm P, Froessler B, Goodnough LT, et al. “Simplified international recommendations for the implementation of patient blood management”. Perioperative Medicine. 2017;6:5. doi:10.1186/s13741-017-0061-8

Leave a Reply